In this post I describe how I would go about using health analytics to identify patients most at risk of an opioid overdose.
The Facts
In 2016, there were 42,249 deaths in the US that involved opioids. That equates to a 13.3/100,000 mortality rate, and approx. one opioid related death every 10 minutes! By the time you finish reading this article, one person probably died of an opioid overdose somewhere in the US.
I will not lament the causes and politics around the opioid crisis. Instead, I’ll describe a scenario in which you, the health analyst, will do an analysis to identify which patients will be approached for opioid overdose prevention programs.
Note: This is a very high level narrative. I will be posting more detailed articles for each of these steps in the near future. Subscribe to receive these.
4 Step Approach
A structured approach to performing analytics is critical to the effectiveness and efficiency of the analysis.
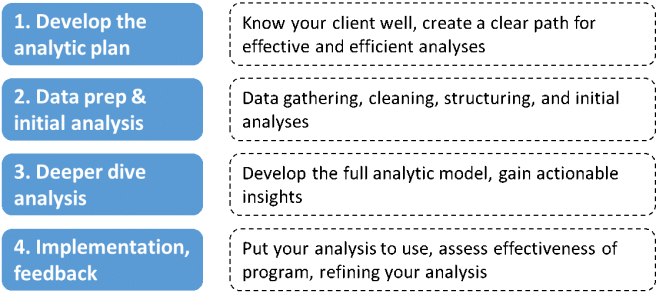
1. Developing the Analytic Plan
Know your client well, develop a clear path for effective and efficient analyses
Having a clear plan improves your effectiveness when you do the analysis, as you will know your objectives for the analysis and what you need to do the analysis. At this step, you also need to seek input from the recipients of the output from the analysis, to learn about their goals, constraints and to ensure what you do is useful.
For the opioid analysis, you’re asked to help the clinical team to identify patients who are most at risk of developing opioid overdose.
You learn from what was done in the past by gathering published research papers on the effectiveness of opioid overdose prevention programs. You succinctly summarize these publications in one page.
You arrange a meeting with the medical director, lead nurse, IT manager and the population health manager. In the meeting, you present the one page of evidence gathered, and get answers to the following questions:
- Why are you doing the analysis? Your analysis will identify patients who could benefit the most from opioid overdose prevention programs.
- For whom? The clinical team, of nurses, doctors, will receive the list of patients most at risk of opioid overdose.
- What kind of interventions? The clinical team will create a series of interventions, including outreach calls, education programs, medication review, behavioral therapy.
- What data do you need vs have? You have EHR data at the clinic, although there might be gaps, such as the lack of prescription fill data.
The Analysis plan
The plan concisely describes the types of data you will need, how you would do the analysis and how the findings will be used. You plan to use EHR data at the clinic to predict a patient’s probability of opioid related overdose over a 1 year period. You will rank all patients by these probabilities. You may also include milestones, timelines and budgets if applicable.
You send the plan to the medical director, my manager/team mates for comments, and update the plan based on their feedback.
Subscribe to receive the detailed post on how to develop the analytic plan.
2. Data Preparation & Initial Analysis
Data gathering, cleaning, structuring and initial analyses
Next, you start gathering the EHR data, through a set of SQL queries. At this step, be careful of the errors in the data as well as the SQL queries. Going wrong here will cost you a lot of time and headache later on.
By checking against other reports and past history, you confirm that the data was correctly pulled and consistent to past experience.
In Excel, you aggregate the data to visualize it and quickly perform some simple analyses. You also find that those patients who had 3 months of prescribed opioids are more likely to continue using opioids, and experience an overdose in the subsequent year. You group the reason for patients being prescribed opioids into 5 categories, including surgery, back pain.
This might be a good time to explore external datasets such as census, public health, income, crime data for the counties that the clinic’s patients live in.
Subscribe to receive the detailed post on how to prepare the data and do the initial analysis.
3. Analysis – Deeper Dive
Develop the full analytic model, gain actionable insights
You discuss findings from your initial analysis with the medical director. She recommends refinements to the patient inclusion, exclusion criteria and suggests a set of clinical logic to identify whether a patient is on opioids appropriately. You refine the SQL code, re-extracts the data and update your analysis. This ensure what you’re doing is clinical correct and that the output will be actionable.
Next, you use statistical methods to identify factors that predict any patient’s probability to develop overdose. You estimate the probability for the patients at the clinic and rank the patients by these probabilities. You use a combination of decision tree, random forest and logistic regression to arrive at a reasonably stable predictive model. You train the model on all patient’s data because the volume of data is relatively low. You also send a few patients to nurses to verify clinically.
You review and write down the methodology, documenting sources of data and assumptions made.
Subscribe to receive the detailed post on how to develop predictive models using health data.
4. Implementation & Feedback
Put your analysis to use, assess effectiveness of program, refine your analysis
You present the finds to the clinical team. The clinical team implements the program for the highest ranked patients.
You provide additional support to the outreach team as necessary, such as patient profiling analytics, optimal time of day to call etc.
At quarterly meetings your review progress and further refine the analysis as needed. At the end of year 1, you will analyze the effectiveness and the return on investment of the program.
Subscribe to receive the detailed post on best practice tips on how to build analyses that are adaptable.
This is a very high level narrative of how one might do an analysis to assist a clinic’s efforts to tackle the opioid crisis. Let me know if you have questions or comments.

3 thoughts on “On Opioids and Analytics”